ADHD Triples the Risk of Substance Abuse: Understanding and Managing Addiction Risk in ADHD Adults
Attention Deficit Hyperactivity Disorder (ADHD) raises the risk of substance abuse: studies show people with ADHD are roughly two to three times more likely to develop addiction. This article summarizes mechanisms linking ADHD and substance use, evidence-based risk factors, and practical prevention and management strategies, with a focus on integrated care and dual diagnosis treatment to support individuals and families.
Key Takeaways
ADHD increases substance abuse risk, often markedly.
Integrated therapy plus medication reduces addiction risk.
Impulsivity and emotional dysregulation are key vulnerabilities.
Mindfulness, exercise, and routine help manage symptoms.
Co-occurring anxiety or depression raises complexity and risk.
Family and community support improve outcomes.
CBT, DBT and MI strengthen coping and engagement.
Dual diagnosis programs improve recovery results.
Effective Management and Prevention Strategies
Reducing substance abuse risk centers on evidence-based, integrated care: combine behavioural therapies, lifestyle changes, and practical supports to improve functioning and lower relapse risk. Key strategies include:
Integrated Treatment Approaches: Medication plus behavioural therapy addresses symptoms and addiction vulnerability.
Building Strong Support Systems: Family and community support provide accountability and encouragement for recovery.
Developing Healthy Coping Mechanisms: Teaching stress management and emotion regulation reduces the need to self-medicate.
Dunham House, a specialized addiction treatment center in Canada, emphasizes integrated, personalized dual diagnosis care for people facing ADHD and substance misuse.
Why Does ADHD Increase the Risk of Substance Abuse?
Core ADHD features, impulsivity, emotional dysregulation and novelty-seeking—raise vulnerability to experimentation and self-medication. People may use substances to modulate attention, mood, or arousal, while impulsive decision-making increases exposure to riskier substance use patterns.
Clinical research consistently identifies impulsivity as a principal factor that elevates the risk of substance use disorders from adolescence into adulthood.
ADHD & SUD Risk in Adulthood: Impulsivity's Role
Adolescents with attention-deficit/hyperactivity disorder (ADHD) face a substantially increased risk of developing substance use disorders (SUD) compared to their peers. Impulsivity, a core symptom of ADHD, contributes to this association and may partially account for higher levels of drug use.
Additional longitudinal and review evidence links high childhood impulsivity with later substance dependence.
Impulsivity as an ADHD-SUD Risk Factor
High impulsivity in children with attention-deficit/hyperactivity disorder (ADHD) is a central factor in their susceptibility to substance use disorders (SUDs). Although impulsivity is recognized as a multidimensional construct, conceptual and methodological inconsistencies have complicated efforts to isolate how distinct impulsivity dimensions contribute to SUD development.
What Are the Evidence-Based Risk Factors Linking ADHD and Addiction?
Research points to several overlapping risk factors that increase addiction vulnerability in ADHD:
Interconnectedness of Disorders: Frequent co-occurrence with anxiety, depression and other conditions increases complexity.
Increased Relapse Risk: Impulsivity and attentional challenges can make sustained recovery harder.
Holistic Care Approaches: Treating ADHD and SUD together yields better outcomes than separate care.
How Do Co-Occurring Disorders Affect ADHD and Substance Abuse Outcomes?
Co-occurring conditions complicate diagnosis and treatment. Anxiety or depression can intensify ADHD symptoms and reduce treatment response unless the full clinical picture is addressed through integrated, concurrent care.
How Can ADHD Be Managed Without Medication to Reduce Addiction Risk?
Non-pharmacological strategies can reduce symptom burden and lower misuse risk. Examples include:
Mindfulness and Meditation: Improve emotional control and reduce impulsivity.
Physical Activity: Regular exercise supports mood and cognitive functioning.
Nutrition and Routine: Structured schedules and healthy eating stabilize daily functioning.
What Non-Drug ADHD Management Strategies Are Supported by Clinical Research?
Lack of sleep triggers ADHD symptoms
Clinical studies support adjunctive, non-drug interventions that aid regulation and functioning:
Art and Music Therapy: Enhances expression and lowers anxiety.
Equine-Assisted Therapy: Supports emotional regulation and social skills.
Sleep Hygiene: Better sleep yields measurable improvements in symptoms.
How Does Behavioural Therapy Help in Managing ADHD and Preventing Substance Abuse?
Behavioural therapies are foundational for both ADHD and SUD prevention. CBT and DBT teach practical coping skills and emotion regulation, while Motivational Interviewing improves engagement and supports sustained behaviour change.
What Are Effective Dual Diagnosis Treatment Approaches for ADHD and Addiction?
Effective dual diagnosis care includes:
Integrated Care Strategies: Coordinated teams of mental health and addiction specialists.
Psychotherapy Options: Tailored therapy that targets both ADHD and substance-related behaviours.
Holistic and Complementary Therapies: Adjunctive approaches to support recovery.
How Does Integrated Dual Diagnosis Treatment Improve Recovery Outcomes?
Coordinated, individualized interventions reduce relapse and improve functioning by addressing ADHD symptoms alongside addiction triggers and coping deficits.
What Role Does Family Support Play in Dual Diagnosis Treatment?
Family involvement strengthens recovery by improving communication, rebuilding trust, and reinforcing treatment strategies; family education and support are often integral to successful outcomes.
What Relapse Prevention Strategies Are Recommended for Individuals with ADHD?
Practical relapse prevention strategies include identifying triggers, strengthening social supports, and maintaining a structured relapse prevention plan tailored to attentional and impulsivity challenges.
Identifying Triggers: Know personal cues and high-risk situations.
Building a Strong Support System: Regular contact with supportive peers, family, or sponsors.
Creating a Relapse Prevention Plan: Concrete steps and coping strategies for high-risk moments.
Which Evidence-Based Techniques Support Long-Term Sobriety in ADHD Patients?
Long-term sobriety is aided by evidence-based therapies, consistent aftercare, and ongoing mindfulness and stress-management practices.
Utilizing Evidence-Based Therapies: Use treatments validated for ADHD and SUD.
Engaging in Aftercare Programs: Continued support after initial treatment is critical.
Practicing Mindfulness: Reduces stress and lowers relapse risk.
How Can Ongoing Education and Support Reduce Relapse Risk?
Continued education about addiction, routine monitoring of mood and substance-use patterns, and sustained access to professional and peer supports empower individuals to make informed decisions and maintain recovery.
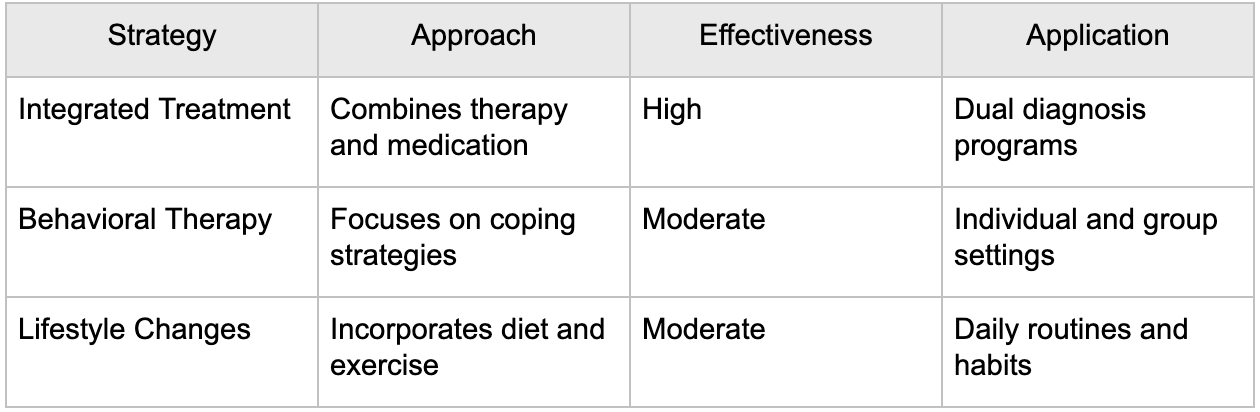
Management strategies for ADHD and substance misuse can be compared by effectiveness and clinical application in the table below.
This comparison highlights the importance of a multifaceted, evidence-based approach to reducing addiction risk in people with ADHD.
Recognizing the link between ADHD and substance abuse is key to prevention and effective care. Integrated, evidence-based treatment plans and robust support systems help reduce risk and improve long-term outcomes.
Conclusion
Understanding how ADHD increases addiction risk enables targeted prevention and treatment. Combining evidence-based therapies, lifestyle supports, family involvement, and integrated dual diagnosis care provides the best chance to reduce substance misuse and support sustained recovery. Seek professional resources and community supports to guide individualized care and long-term well‑being.
Dunham House specializes in true concurrent dual diagnosis care, recognizing that addiction rarely occurs in isolation. A critical component of this specialization is addressing common co-occurring mental health disorders like Attention-Deficit/Hyperactivity Disorder (ADHD) alongside substance use disorder. By treating the underlying ADHD as an integral part of the addiction, the program ensures that the core psychological and neurobiological drivers of self-medication are managed effectively, leading to more stable and long-term recovery outcomes. This integrated approach, which treats the whole person, is a key differentiator from facilities that treat these conditions sequentially.
Dunham House
About Dunham House
Located in Quebec's Eastern Townships, Dunham House is a residential treatment centre specializing in addiction and providing support to individuals with concurrent mental health challenges. We are the only residential facility of our kind in Quebec that operates in English.
Our evidence-based programs include a variety of activities such as art, music, yoga, and equine-assisted therapy. In addition to our residential services, we offer a full continuum of care with outpatient services at the Queen Elizabeth Complex in Montreal.